There is a lot for you to think about when choosing the best way to treat or manage your cancer. There may be more than one treatment to choose from. You may feel that you need to make a decision quickly. But give yourself time to absorb the information you have learned. Talk to your doctor. Look at the list of "Questions to Ask Your Doctor" to get some ideas. Then add your own.
It is often a good idea to get a second opinion, especially from doctors experienced in treating breast cancer. A second opinion can provide more information and help you feel more secure about the treatment plan you choose. Some insurance companies require a second opinion before they will agree to pay for certain treatments. Almost all will pay for the second opinion.
This is a brief summary of the types of treatments used for breast cancer. The American Cancer Society also has more detailed information about breast cancer treatment options available through our toll-free number or on our Web site. Of course, your doctor may have reason to suggest a treatment plan different from these general guidelines. So don't hesitate to ask questions and to seek out information about treatment from other reliable sources.
Each type of treatment has benefits and drawbacks. There may be side effects. Your age, your overall health, and the stage of your cancer are all factors to take into account.
If you would like to talk to another woman who has had breast cancer, we encourage you connect with a volunteer in our Reach to Recovery program. A specially trained volunteer can provide information, comfort, and support. To learn more about Reach to Recovery or to request a visit, please call us at 1-800-ACS-2345.
Local vs. Systemic Treatment
The purpose of local treatment is to treat a tumor without affecting the rest of the body. Surgery and radiation are examples of local treatment. Systemic treatment is given into the bloodstream or by mouth to reach cancer cells that may have spread beyond the breast. Chemotherapy, hormone therapy, and immunotherapy are systemic treatments.
When people who seem to have no cancer after surgery are given more treatment it is referred to as adjuvant therapy. Doctors now think that cancer cells can break away from the main tumor and begin to spread through the bloodstream in the early stages of the disease. It’s very hard to tell if this has happened. But if it has, the cancer cells can start new tumors in other organs or the bones. The goal of adjuvant therapy is to kill these hidden cells.
Some people are given systemic treatment (most likely chemotherapy) before surgery to shrink a tumor. This is called neoadjuvant therapy.
Types of Surgery for Breast Cancer
Most women with breast cancer will have some type of surgery to treat the main breast tumor. The purpose of surgery is to remove as much of the cancer as possible. Surgery can also be done to find out whether the cancer has spread to the lymph nodes under the arm (axillary dissection), to restore the breast's appearance (reconstructive surgery), or to relieve symptoms of advanced cancer. Here is a summary of some of the most common types of breast cancer surgery:
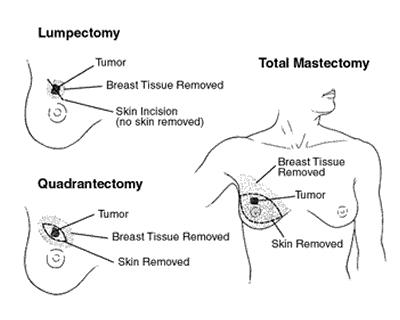
Lumpectomy (lump-EK-tuh-me): Also called breast conservation therapy, lumpectomy involves removing only the breast lump and some normal tissue around it. Radiation treatment is often given for about 6 weeks after this type of surgery. If chemotherapy is going to be used as well, the radiation may be postponed until the chemo is finished.
Partial (segmental) mastectomy (mas-TEK-tuh-me): This surgery involves removing more of the breast tissue than in a lumpectomy. It is usually followed by radiation therapy.
Simple or total mastectomy: In this surgery the entire breast is removed but not the lymph nodes under the arm or muscle tissue from beneath the breast.
Modified radical mastectomy: This operation involves removing the entire breast and some of the lymph nodes under the arm.
Radical mastectomy: This is extensive removal of entire breast, lymph nodes, and the chest wall muscles under the breast. This surgery is rarely done now because modified radical mastectomy has proven to be just as effective with less disfigurement and fewer side effects.
Choosing Between Lumpectomy and Mastectomy
One advantage of lumpectomy is that it saves the way the breast looks. A downside is the need for several weeks of radiation after surgery. But some women who have a mastectomy will still need radiation. For most women with stage I or II breast cancer, lumpectomy or partial mastectomy (along with radiation) is as good as mastectomy. There is no difference in the survival rates of women treated with these 2 methods. Other factors, though, can affect which type of surgery is best for you. And lumpectomy is not an option for all women with breast cancer. Your doctor can tell you if there are reasons why a lumpectomy is not right for you.
Possible side effects of mastectomy and lumpectomy include infection and blood or fluid collecting at the place where the incision is made. If lymph nodes are removed, there could be other side effects as well such as swelling of the arm (lymphedema).
Other Breast Cancer Surgeries
Axillary dissection: This operation is done to find out if the breast cancer has spread to lymph nodes under the arm. Some nodes are removed and looked at under a microscope. Knowing whether there are cancer cells in the lymph nodes can help guide other treatment decisions.
A possible side effect of removing these lymph nodes is swelling of the arm, called lymphedema. It happens to about 10% to 30% of women who have had these nodes removed. Women who have swelling, tightness, or pain in the arm after lymph node surgery should be sure to tell their doctor right away. Often there are measures to prevent or reduce the effects of the swelling. The American Cancer Society has more information about lymphedema available through our toll-free number or on our Web site.
Sentinel lymph node biopsy: This is a way to look at the lymph nodes without having to remove all of them first. For this test, a radioactive substance and a dye are injected near the tumor. They are carried by the lymph system to the first (sentinel) node to receive lymph from the tumor. This lymph node is the one most likely to contain cancer cells if the cancer has spread. Once this node is found, it is removed and examined. If the sentinel node contains cancer, more lymph nodes are removed. If it is free of cancer, further lymph node surgery might not be needed. This type of biopsy is complex, so it is best to have it done by experts who have a lot of experience in doing it.
Reconstructive or breast implant surgery: These operations are not meant to treat the cancer but are done to restore the way the breast looks after mastectomy. If you are having a mastectomy and are thinking about having reconstruction right away, you should talk to a plastic surgeon before your operation. There are several choices about when the surgery can be done and exactly what type it will be.
You can get more detailed information about each of these types of surgery and their possible side effects available through our toll-free number and on our Web site. Ask for "Breast Reconstruction After Mastectomy." Also, you might find it helpful to talk to a Reach to Recovery volunteer who has had the method you’re thinking about.
What to Expect with Surgery
For many women, the thought of surgery can be frightening. But a better understanding of what to expect before, during, and after the operation may help ease your fears.
A few days after your biopsy you will know whether or not you have cancer, but the extent of the disease will not be known until after surgery. You will most likely meet with your surgeon a few days before the operation to talk about what will happen. You will be asked to sign a consent form giving the doctor permission to do the surgery. This is a good time to ask any questions you might have.
You may be asked to donate blood ahead of time in case you need it during the surgery. Your doctor will also ask you about medicines you are taking. You might need to stop taking some of them a week or two before surgery.
The type of anesthesia you will have depends largely on the kind of surgery being done and your own situation. How long the surgery will take and how long you will be in the hospital also depends on the type of surgery you are having.
As a rule, women having a mastectomy stay in the hospital for 1 or 2 nights and then go home. Lumpectomy and sentinel lymph node biopsy are usually done on an outpatient basis and do not require an overnight stay in the hospital.
After surgery you will have a bandage over the surgery site. You may have one or more tubes (drains) from the breast or underarm area to remove fluid that collects during the healing process. Most drains stay in place for a week or two. Once the flow has gone down to about one ounce a day, the drain will be removed.
Most doctors will want you to start moving the arm soon after surgery so that it won’t get stiff. Women who have a lumpectomy or mastectomy are usually surprised by how little pain they have in the breast area. But they are less happy with the strange feelings (numbness, pinching/pulling) in the underarm area.
Talk with your doctor about what you should do after the surgery to care for yourself. You’ll probably get written instructions that will tell you about the following:
how to take care of the wound and dressing
how to take care of the drains
how to know if you have an infection
when to call the doctor or nurse
when to begin using the arm and how to do arm exercises to prevent stiffness
when to start wearing a bra again
when and how to wear a breast form
what to eat and what not to eat
what medicines to take (including pain medicines)
what activities you should or should not do
what feelings you might have about how you look
how to contact a Reach to Recovery volunteer. These specially trained women can provide information, comfort, and support.
You will see your doctor a week or two after surgery. He or she should explain the results of your pathology report and talk to you about whether you will need further treatment.
Chemotherapy
Chemotherapy is the use of anticancer drugs injected into a vein or taken as a pill. These drugs enter the bloodstream and reach throughout the body, making the treatment useful for cancers that have spread to distant organs. While these drugs kill cancer cells, they also damage some normal cells, which can lead to side effects.
If chemotherapy is given after surgery it can reduce the chance of breast cancer coming back. Chemotherapy can also be used as the main treatment for a woman whose cancer has already spread outside the breast and underarm area or that spreads widely after the first treatment.
Chemotherapy may be given before surgery, often to shrink the tumor in order to make it easier to remove. This approach also allows the doctors to watch how the tumor responds to the drugs. If the tumor does not shrink, different drugs can be used.
Chemotherapy is given in cycles, with each period of treatment followed by a break. The total course of treatment usually lasts about 6 months. Often several drugs are used together rather than a single drug alone.
The side effects of chemotherapy depend on the type of drugs used, the amount given, and the length of treatment. You could experience some of these temporary side effects:
being very tired (fatigue, caused by a shortage of red blood cells)
nausea and vomiting
loss of appetite
hair loss
mouth sores
changes in menstrual cycle (this could be permanent)
a higher risk of infection (from a shortage of white blood cells)
bruising or bleeding after minor cuts (from a shortage of blood platelets)
Most of these side effects go away when treatment is over. For example, your hair will grow back. If you have any problems with side effects, be sure to tell your doctor or nurse because there are often ways to help.
Permanent side effects can include early change of life (menopause) and not being able to become pregnant. Heart damage can occur if the drug Adriamycin is used for a long time or in high doses, but doctors are careful to control the dose of this drug and to watch for signs of problems.
Also, many women who have had chemotherapy notice a slight decrease in concentration and memory. This may last a long time.
Very rarely, years after treatment for breast cancer, certain chemotherapy drugs may cause another cancer called acute myeloid leukemia. But the benefit of treating the breast cancer far outweighs the risk of this rare event.
Lastly, many women do not feel as healthy after having chemotherapy as they did before. There may be pain and a mild loss of physical functioning.
Radiation Therapy
Radiation therapy is treatment with high-energy rays (such as x-rays) to kill or shrink cancer cells. The radiation may come from outside the body (external radiation) or from radioactive materials placed directly in the tumor.
Most often, external radiation is used for treating breast cancer. It is much like getting a regular x-ray but for a longer period of time. Radiation therapy may be used to destroy cancer cells remaining in the breast, chest wall, or underarm area after surgery or- less often-to reduce the size of a tumor before surgery.
Treatment is usually given 5 days a week in an outpatient center over a period of about 6 weeks, beginning about a month after surgery. Each treatment lasts a few minutes. The treatment itself is painless. If it is used along with chemotherapy, radiation is usually given after chemotherapy is finished.
The main side effects of radiation therapy are swelling and heaviness in the breast, sunburn-like changes in the treated area, and possibly fatigue. These changes to the breast tissue and skin usually go away in 6 to 12 months. In some women, the breast becomes smaller and firmer after radiation therapy. Radiation therapy is not given during pregnancy because it can harm the fetus.
Another way to give radiation is to place radioactive seeds (pellets) into the breast tissue next to the cancer. It may be given to add an extra “boost” of radiation to the tumor. It is also being studied as the only source of radiation. So far the results have been good, but more study is needed with this method before it can be used as standard treatment.
Hormone Therapy
The female hormone estrogen promotes the growth of breast cancer cells in some women. For these women, several methods to block the effect of estrogen or to lower its levels are used to treat breast cancer.
A drug such as tamoxifen, which blocks the effects of estrogen, can be given to counter the effects of estrogen. Tamoxifen is taken in pill form, usually for 5 years after surgery, to reduce the risk the cancer will come back. Recent studies have clearly shown that this drug helps women of all ages with early breast cancer if their cancer has estrogen receptors. It is also used to reduce the risk of breast cancer in women who are at high risk.
Some studies have shown an increase of early stage cancer of the lining of the uterus among women taking tamoxifen. But this cancer is usually found at a very early stage and is almost always cured by surgery. Tell your doctor right away if you have any unusual vaginal bleeding. Blood clots are another possible side effect of tamoxifen. Others can include hot flashes and mood swings. Still, for most women with breast cancer, the benefits of tamoxifen far outweigh the risks.
Aromatase inhibitors are a type of drug that stops the body from making estrogen. They only work for women who are past menopause and whose cancers are hormone positive. These drugs may be used after, or even instead of, tamoxifen to reduce the risk of the breast cancer coming back. They don’t cause uterine cancer and very rarely cause blood clots. They can, however, cause bone thinning and fractures because they remove estrogens from the body.
There are several other drugs that affect female hormones which are being used for breast cancer. Your doctor can give you more details about any recommended treatments.Other Treatments
Trastuzumab (Herceptin) is a drug that attaches to a growth-promoting protein (HER2/neu) that is found in small amounts on the surface of normal breast cells and most breast cancers. Some breast cancers have too much of this protein, which can cause the cancer to grow and spread faster. Herceptin can stop this protein from causing breast cancer cell growth. It may also help the immune system to better attack the cancer.
Herceptin is most often started after standard hormonal or chemotherapy is no longer working, but studies are going on now to see if it should be added to the first course of chemotherapy. The side effects of this drug are fairly mild. They may include fever and chills, weakness, nausea, vomiting, cough, diarrhea, and headache. But some women have heart damage during treatment. If you are having this treatment, you should tell your doctor right away if you have any shortness of breath or trouble with physical activities.
Two drugs (bisphosphonates) that help strengthen bones are in use. They are given into a vein to help prevent bone damage if the cancer has spread to the bone. There are also some studies in progress to see if these drugs can prevent spread to the bone.
In the past, it was thought that very high doses of chemotherapy followed by a method called stem cell transplant might offer some women with a high risk of the cancer coming back or with advanced cancer the best chance for a cure. But doctors have found that the women who received high dose therapy did not live any longer than women who had standard dose chemotherapy. And high dose chemotherapy with stem cell support can cause serious side effects. Research in this area is still going on. For now, experts in the field suggest that women receive this treatment only as part of a clinical trial.
American Cancer Society website: http://www.cancer.org